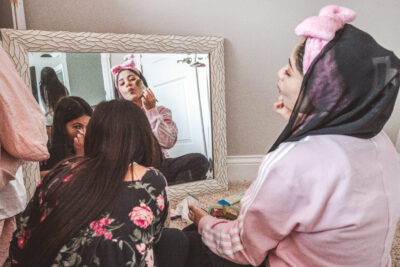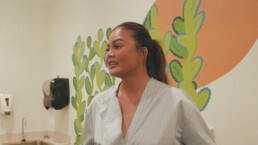The Toni Morrison approach to mothering
Black women deserve to claim and relish the depths of freedom motherhood can bring.
By Rebecca Carroll
When I was nursing my son as a baby, he started doing this thing where he would latch the little fingers of his free hand around my bottom lip, and then proceed to slowly knead at it in a small but persistent effort to pry open my mouth. It almost felt like he was trying to find some sort of entryway back into my body. Once, when he was about two, I softly placed my hand over his as he tugged at my lip, and asked in a whisper, “Does this feel like love to you?” He stared back at me with his beautiful, bright eyes, and nodded “yes.” It felt like love to me, too.
I am reminded of this hushed exchange of heartwork between us whenever I see one of these pieces about “styles of parenting” that crop up online every now and again, introducing or reintroducing terms like “attachment parenting,” “helicopter parenting,” “gentle parenting,” and “intensive parenting.” The methods they describe might sound fresh, but they’re often adjacent to the four Mayo Clinic-approved styles of parenting, which have been around since the 1960s—authoritative, authoritarian, permissive, and uninvolved. And they almost always feel white-coded, not just because labeling (or, let’s be honest, marketing) how parents interact with their children is about having the time and the income to ponder how you might like to categorize your “style” of parenting. These terms also dissociate and intellectualize what is, to me, and to many Black mothers I know, an emotionally freeing, visceral experience.
It is striking to me how little the experience of Black mothers factors into the standard offerings on how to parent today. Instead, we get media portrayals of Black mothers as struggling single moms and “modern-day mammies,” or neck-rolling, meme-friendly, “You got McDonald’s money?” kinds of stereotypes. But Black mothers are, and Black mothering is, so much more than that. And we deserve to claim and relish the depths of freedom mothering can bring——especially given the inherent, deeply harrowing history of when and if we were even able to keep our children.
Morrison offers this piece of advice: “When they walk in the room, my face says I’m glad to see them.”
No one knew that better than the late novelist Toni Morrison, who was herself a single mother of two boys. Becoming a mother, Morrison said in a 1989 conversation with Bill Moyers, “ was the most liberating thing that ever happened to me.” The demands of her children, she went on to explain, were not like those of her colleagues, friends, or lovers. “Somehow all of the baggage that I had accumulated as a person about what was valuable just fell away. I could not only be me—whatever that was—but somebody actually needed me to be that.” That’s exactly how I felt when I was nursing my son, when he needed me to be that person who would feel like love.
Later, years after I stopped nursing, I snuggled him often and regularly, let him sleep in the bed with us at night, and made myself available to him in ways that felt centered and honest. I seldom missed a call. I always allowed myself to be vulnerable even, and especially, when I didn’t have an answer to solve a problem—while also trying like hell to solve the problem. “If you listen to [your children],” said Morrison, in that same conversation with Moyers, “somehow you are able to free yourself from baggage and vanity… and deliver a better self, one that you like. The person that was in me that I liked best was the one my children seemed to want.” Obviously, we have to make choices, set boundaries, and act as moral compasses for our children, but isn’t that part of delivering the version of ourselves that we like best?

REBECCA AND HER SON, KOFI (COURTESY OF REBECCA CARROLL)
My friend Caryn and I raised our sons, who are just eight months apart, as cousin-brothers, and have frequently mused over the past 21 years about the ways in which parenting Black children is not just about “the talk” for our sons, or warnings about the oversexualization of Black girls for our friends with daughters. It’s about mitigating the harshness of their inevitable reality growing up in America, with the softness of our generational instincts.
Morrison’s approach to parenting squarely challenges the meme and media stereotypes (not that she would have paid them much mind), and blatantly disregards white mainstream guides. Black mothering doesn’t need a name or a category; it deserves a kind of reverence. In simpler terms, Morrison offers this one piece of salient advice: “Let your face speak what’s in your heart. When they walk in the room, my face says I’m glad to see them. It’s just as small as that, you see?”
The summer after my son went to college, I was really struggling with him being away. Like, actually grieving. We sat down one evening to talk about it. I told him how hard it was for me to be physically separated from him, almost as if a part of my body was missing. And he said, “Mom, I’m doing what I’m supposed to be doing. And that’s a testament to you and your mothering.” I’d like to think that is in no small part because my face has always said I’m glad to see him when he walks into a room.
More Mother’s Day reading and watching from The Meteor:
A Feminist Love Letter to Baby Formula
It’s Time to Rethink the Empty Nest
My Abortion Story Is Not What You Think
Three Questions For Tracy Clark-Flory About Motherhood and Sisterhood
Syria's Mothers Are Fighting to Rebuild Their Homes
The Women Who Exposed the "Rape Academy"
Three journalists tell the inside story of investigating a dark global network of men assaulting their partners
By Nona Willis Aronowitz
On March 26, CNN published a 16-minute documentary and interactive story about “a global rape academy,” a network of websites and Telegram chat where men trade tips on how to drug and sexually assault their wives and girlfriends. The story has since been viewed and read by millions, first across Europe and then in the U.S., where the story went viral a few weeks later. Behind the exposé were nearly 25 CNN journalists and staff who for seven months dug into this vast and tightknit community. The Meteor spoke with investigative reporters Saskya Vandoorne and Niamh Kennedy, and reporter and producer Kara Fox, about how this extraordinary investigation came together.
Saskya Vandoorne: It all started with Gisèle Pelicot. I'm the CNN Paris bureau chief here, and I was at the trial down in the south of France [in the fall of 2024] where 51 defendants were on trial for raping her. And I remember very vividly her lawyer speaking about Coco, the platform that Dominique Pelicot had used to recruit all these men to rape his sedated wife. The lawyer described Coco as the weapon of the crime. He said Pelicot had gone on there to find like-minded people. So even though Coco had been taken down, I was curious to find out: Are there any other spaces where men speak to one another about crimes they wanted to commit against their wives or partners?
Kara Fox: We had been reporting out the Dominique Pelicot case, and we knew that Coco users were talking about where to go next on a forum. As we knew that these spaces didn’t go away after the trial, we investigated some of them—other websites and a large Telegram group. One site in particular became the focus, also reported on through the amazing work of German journalists Isabel Beer and Isabel Ströh: Motherless.com. Throughout the course of our reporting we also reported on similar cases, like “the German Pelicot” or “the UK Pelicot.”
Niamh Kennedy: [In the “sleep” groups on] Motherless, there were over 20,000 videos, some showing unconscious women and their eyelids being lifted up to show that they've been sedated. There were more graphic videos as well, sometimes showing what appeared to be nonconsensual sex acts being carried out on these sedated women. It was from spending a lot of time on Motherless that I found a link to the private Telegram group [called “Zzz”]. It featured 1,000 men from all around the world who were giving each other tips on how to drug and rape their partners. It was quite tough, to be honest with you…I definitely felt chills a lot of the time seeing what was going on there. It was very hard.
An upside-down world
SV: There were many conversations that were had before we went undercover [to log onto the site and join the Telegram group to speak to participants]: What did we want to achieve? What could we say? Where was the line? We wanted to remain journalists, so our role was just to ask questions. At no point did we want to encourage any of this behavior; of course, we weren't going to share any pictures or videos of our fictitious wives. So it was very much, sit in this space, ask questions, find out what are they doing, how long have they been doing it for. And also, what was their motivation?
NK: Saskya and I made a shared fake profile, working late into the evening when a lot of the men were online. We spent a lot of time both on the site and in the private Telegram group. There were tiers: men who were selling content, men who were selling sleep liquids—very powerful drugs that could immobilize women. There were men that were offering livestreams. We're talking about hundreds of messages all day long, ping pong, ping pong. They would turn to each other for advice. One guy would write in and be like, "I'm thinking of drugging and raping my wife. Who's done this before?" And one guy would be like, "Yep, I've been doing this for three years. Use this drug." Others would be like, “What weight is she?” “Oh, I did this and I got away with it. " And then a couple of hours later, the man who'd asked the question would post a video and they'd be encouraging each other. It was like a whole brotherhood, where they were really bonding over this shared interest.

SV: [There, the] world is turned upside down. In our world, you've got Gisèle Pelicot, a feminist idol. On Motherless, it's Dominique Pelicot who is the idol. They see him as some kind of god to revere and to emulate.
KF: These users are very comfortable and callous and boisterous. They're not afraid to say what they're doing. They appear to be living in this place where they think they're immune. The psychologist that evaluated half of the men in the [Pelicot] trial told us that they feed on this collective energy of not just the excitement around the abuse, but also allowing themselves to normalize it.
SV: [In the groups] there's this feeling that your wife, your girlfriend, is yours. She is your object to possess, and therefore, it's not rape because you know her, because you're having sex with her anyway. I remember one man said, "Well, I'm not cheating on her. I'm still having sex with her, so she should feel lucky.”
Another way of understanding their mindset is a pendulum swing: Is it because of the emancipation of women, that women are now independent and they have power? Do these men feel under threat? Do they feel like this is a way of getting back the control of being once again the dominant alpha male? Because there is nothing more dominant than a man performing sex acts on an inanimate woman's body. I felt that was fueling some of this behavior.
“A complete shot in the dark”
SV: A lot of the men we met in the Telegram group would get very suspicious [of our questions] and the conversations would go cold. But there was this one Polish man, whom we call Piotr in the piece, who was willing to talk and was happy with me being a sounding board, just listening to him and asking questions. I think he was lonely and just really needed to talk. He assumed that I was someone who shared the same fantasies as him, and he was incredibly trusting. And so he would talk about what he was up to that weekend, the holidays he'd go on with his wife and the social activities he would do with his friends. It wasn't all darkness.
One day, Piotr let it slip that he was going to a party at a restaurant.
NK: The thing that made this experience feel more real was when we traveled to Poland to track down Piotr [to confirm that he was real]. He didn’t give us the name of the restaurant, and there was no guarantee that we would find the right place. We were piecing together cryptic clues. We'd figured out based on a photo where he lived, geolocated his house, and then it was just internet research going through all the different restaurants in the area. We found one that had an event which matched the criteria that he'd mentioned. It was a complete shot in the dark.
SV: I remember the party was meant to start at 7:00 and everyone had arrived by 7:05. [Piotr and his wife] still weren't there. I sent a message to Niamh who was standing across the road: "This is the wrong place. They're not going to be here tonight." And then they came out of the car.
NK: When we saw him face-to-face, my heart sank because it's almost like I didn't want it to be true. But everything matched up: the facial identities, the people. He hadn’t been lying.

SV: What was even worse than seeing him was seeing her. Because I'd seen many photos and videos of her. You are a journalist, you're not there to interfere, but I remain a woman. So of course you can't help but think if the shoe was on the other foot, if I were her and she were me, would I want [a journalist] to come and tell me right there and then? And so it was really chilling, unnerving. It was almost a kind of out-of-body experience. I felt like I was watching the scene from up above, and I had to slightly dissociate from my emotions to be able to continue working as a journalist.
Seeing them on the dance floor was also a pretty harrowing moment: She would be dancing with her friends, he would come to join her, and she would leave and sit back down. You just felt that she was kind of fleeing him. Her face had such a vacant expression. This is me projecting, but it was almost as if her body knew what he was doing to it. It was a very strange and cold dynamic.
NK: We're not police officers, but in this case, we felt that we had to do a little bit more [than just observe]. Saskya and I made the call not to approach them because we were very mindful of this woman and her safety, but we did hand our findings in to the police. They were incredibly responsive. [On April 9, Polish authorities confirmed that] they arrested him and he's admitted to all the charges.
SV: We knew the Piotr meeting would be the final stage of the investigation because as soon as we had confirmed who he was, we weren't going to sit on that. So before we got to that stage, we had made sure that we had checked out all the other survivors’ stories that we were going to weave in.
NK: The thing that really brought it all to life was meeting women who, though they weren't directly connected with this group, were survivors of this kind of abuse. The men in this group felt very invisible; they had these shadowy personas. And then when we met people that had been impacted by this kind of harm, that…made it all feel so real. Although I was in awe of their bravery, I was also deeply, in my soul, devastated to see the impact of this.

“A question of whack-a-mole”
KF: The arrival of publication day was a collective exhale. There's been a viral outpouring from survivors; they're flooding our inboxes with stories. Even for us, who know that this sort of abuse has been going on, to see so many survivors coming from the U.S., Australia, Europe, the UK is a lot. And we've seen people talking about their own rape stories and naming their rapists—not necessarily rape that had to do with [drug-facilitated sexual assault], but they felt like this was a moment to reclaim their own narratives.
SV: People began to understand that Dominique Pelicot is not an outlier. He's not unique. This is a phenomenon, and that's why we need to take note of it. The algorithms need greater scrutiny: Some of these guys may be going onto a porn site just watching regular porn, but then they find this slightly darker corner of this website where they're like, "Oh, what is ‘sleep porn’? This is interesting. This is forbidden. Maybe I'll try it out." It is out there, it's not on the dark web, it's easily accessible.
KF: [From a legal standpoint] it looks like there's momentum. In Europe, for example, there's legislation that's being proposed about non-consensual sex and how to define it from a yes-means-yes perspective instead of what exists right now. Several members of the European parliament raised our investigation as proof that more needed to be done. [A majority of the European Parliament approved the “only yes means yes” rape definition on April 28, in order to close any existing loopholes in rape legislation. Irish MEP Maria Walsh said that CNN’s investigation accelerated the debate.]
SV: [We need] more awareness of red flags. We need to ensure that the next time a woman goes to see her doctor and starts complaining about fuzziness or not remembering things she did last week, that if her husband is sitting next to her, the doctor might say, "Hey, can I have a moment alone with you?” So many of these women would go into the doctor's office with their husband, who would then manipulate the conversation like, "Hey, you've been under a lot of pressure, a lot of stress." And police need to recognize that drug-facilitated abuse [happens with] couples in marriages.

Of course, there needs to be better moderation and regulation. In the wake of our investigation, there has been a public outcry here [in France] about Cocoland, [a new site] which has the same interface and is modeled completely on Coco. Just today, prosecutors opened an investigation into this website. But even though the Coco founder has been charged, he's not in custody, and the trial is not set to take place for another year or two. Even today, if you were to go on Motherless, you would still be able to find sleep-content videos on there. So yes, better moderation, but also maybe harsher sentences and real legal repercussions when it comes to these founders. Because let's say tomorrow Motherless is taken down. What's to stop five other websites taking its place? It’s a question of whack-a-mole.
The last thing I’ll say is that if people want these kinds of investigations to see the light of day, you need well-funded news organizations. When [you include] the cameramen, the editors, the people who built the interactive, the lawyers, we were about 25 journalists who worked on this in the end. You need the time, the infrastructure to be able to produce this kind of investigation. The more we can raise awareness, the greater chance we have of survivors feeling like they're not alone and of spurring actual change.
So far, Motherless doesn't appear to have banned the so-called “sleep content,” although some related search terms or tags seem to have disappeared since the publication of CNN’s investigation. Meanwhile, other search terms still lead users to what appears to be drug-facilitated sexual assault content. The Zzz Telegram group has vanished from the Telegram chat list, but Telegram has not responded to CNN's questions about the disappearance.
Is ICE a reproductive health hazard?
 April 17, 2026 The “Toxic Legacy” of Operation Metro SurgeThis winter, in Minnesota and elsewhere around the country, ICE used tear gas on citizens. Now public health experts worry that these chemical weapons may be linked to reproductive problems. Yessenia Funes reports.BY YESSENIA FUNES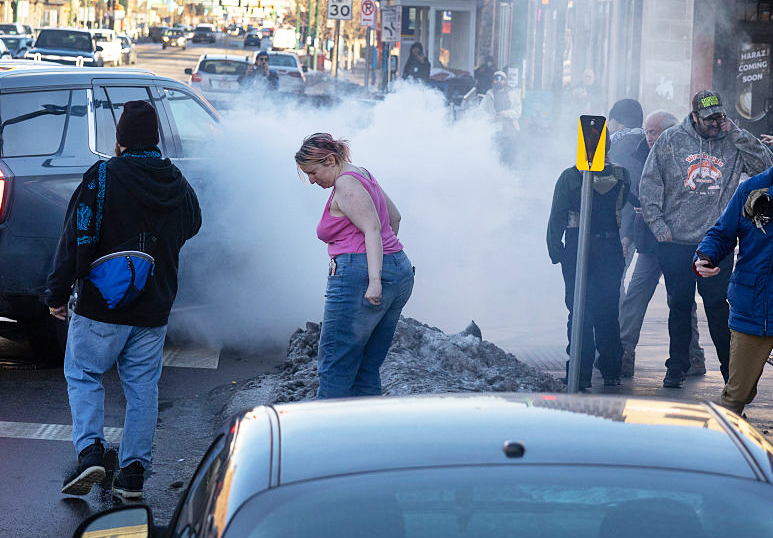 TEAR GAS ON A STREET IN MINNEAPOLIS THIS WINTER. EVEN THOSE NOT PROTESTING WERE AFFECTED, RESIDENTS SAY. (PHOTO BY SCOTT OLSON/GETTY IMAGES.) Asha kept a bag ready throughout most of January and February. Inside, she packed bandages, gauze, water, saline, tourniquets, and general first aid. The 30-year-old works as a healthcare professional in Minneapolis, and when she’s off the clock, she responds to community emergencies as a street medic, mostly treating her neighbors who have been exposed to chemical weapons. On the day in January when federal officers shot and killed 31-year-old nurse Alex Pretti, she says, “I watched a lot of elderly people get tear-gassed.” And that wasn’t the first or the last time Asha, who is sharing only her first name to protect her identity, saw law enforcement attack her neighbors. Since the Trump administration’s Operation Metro Surge, which deployed 3,000 federal immigration agents to the Twin Cities, the emergencies have felt nonstop to Asha. The administration concluded its Minnesota incursion on Feb. 12, firing Homeland Security Secretary Kristi Noem weeks later, partly for her failure to manage the fallout in the state. Minneapolis is seeing fewer agents than in prior months, but people are still scared. And the whole city still feels the surge’s effects in their bodies—perhaps literally. Public health experts fear that ICE’s actions will leave a toxic legacy for communities across the country. In cities like Los Angeles, Portland, and Washington, D.C., independent analysts have raised concerns over federal officers’ indiscriminate deployment of chemical agents like tear gas or pepper spray—and not just on protesters. People are being exposed while stepping out for work or errands, or even sometimes at home. Researchers can’t easily study the long-term impacts of these weapons—there’s no ethical way to expose people to these chemicals in a controlled experiment—but what they do know paints an alarming portrait for public health, especially in women, people with uteruses, and children. Asha Hassan, an assistant professor of women’s health at the University of Minnesota Medical School (not to be confused with the street medic), began collecting data on reproductive health impacts in 2020 when the Black Lives Matter uprisings sprang up across the country and, with them, a police response that often involved tear gas. She had heard whispers of menstrual irregularities and miscarriages, but after looking at the available literature, she realized scientists had ignored some key population groups. “A lot of the research that we do have on tear gas is from the ’50s and ’60s,” Hassan explains. “It’s on mostly healthy men who are in a military setting. It really hasn’t been tested on women, children, people with chronic conditions, people with any sort of disability.” Studies have focused on “this particular type of body: a cis, straight man who is serving in the military and has the ability to be healthy.”  A PROTESTER IN LOS ANGELES FLUSHES A FELLOW DEMONSTRATOR’S EYES OUT AFTER EXPOSURE TO TEAR GAS. (PHOTO BY JON PUTMAN/ANADOLU VIA GETTY IMAGES After putting out a social media call to hear from those who had been exposed to chemical weapons like tear gas, she received more than 600 emails from all over the world in just a few weeks. In 2023, she published a paper that included more than 1,200 responses from people exposed in the U.S. between 2020 and 2021. The findings confirmed Hassan’s fears: Tear gas exposure was linked to negative reproductive health impacts for anyone of reproductive age. “Even after one exposure, we started to see some impact,” she says.
The more a person had been exposed, the more likely they were to face a number of issues: breast tenderness, spontaneous bleeding, and cramping. The study also found an above-average rate of miscarriages, but the sample size didn’t include enough pregnant participants to make a strong conclusion about tear gas’s effect. AN “OBJECTIVELY CHILLING” USE OF TEAR GASIn the decades after World War II, the majority of world leaders agreed to ban riot control agents during war as part of the Chemical Weapons Convention. (The U.S. government shares limited information on the chemicals that make up these weapons, but they can include chlorobenzylidene malononitrile and dibenzoxazepine, which can harm the respiratory system.) However, U.S. police are still allowed to use these weapons to protect public safety, explains Rohini Haar, a public health professor at U.C. Berkeley and medical adviser at Physicians for Human Rights. But that’s not what’s happening in the U.S. under Trump, Dr. Haar believes. “You’re not seeing that these weapons are used to quell any sort of riot or protect public safety,” Dr. Haar says, emphasizing that ICE agents have fired tear gas as protesters were walking away, not to disperse a crowd. “They’re actually harming public safety.” Dr. Haar has treated tear gas patients across the globe, including at the Aida Refugee Camp in the West Bank. There, Palestinian families have been exposed to periods of near-daily tear-gas use by Israeli soldiers. No one is safe—not people cooking dinner at home or children walking to school. “That’s happening now in the U.S., too,” Dr. Haar says. “The experience in Aida is kind of a warning.” Indeed, a federal judge ordered ICE to stop its use of tear gas in Oregon last month after the American Civil Liberties Union filed a lawsuit on behalf of protesters. In his filing, U.S. District Court Judge Michael Simon wrote, “Defendants’ conduct – physically harming protesters and journalists without prior dispersal warnings – is objectively chilling.” At least one additional case also focuses on the federal government’s recent use of chemical weapons in Portland. The Meteor reached out to Customs and Border Protection to understand its reasoning behind officers’ liberal use of tear gas. The agency did not comment, but Gregory Bovino, the ICE official who led the Minnesota operation and lost his job in January, has defended the use of chemical weapons as a favorable alternative to “lethal devices.” In Minneapolis, ICE agents have also deployed tear gas outside people’s apartments and buildings, where the chemicals can and do seep indoors. The weapons are most toxic in enclosed spaces. The day officers killed Pretti, Asha, the street medic, fled into an apartment building to catch a break. “The air inside was almost as bad as the air outside,” she recalls. “You were standing inside and coughing,” Asha says. Tear gas “was seeping into every apartment in that hallway.”  PEOPLE IN MINNEAPOLIS RUN FROM TEAR GAS—WHICH FEDERAL AGENTS USED WIDELY THE DAY THEY KILLED NURSE ALEX PRETTI. (PHOTO BY STEPHEN MATUREN/GETTY IMAGES) For those who aren’t familiar with the chemicals, stepping outside of one’s home can feel completely normal—until the stinging, dry stench hits, explains Minneapolis resident Slime Seamstress, a 31-year-old trans seamstress using their soon-to-be legal name. They were exposed to tear gas twice in January. They never attended a protest; exposure occurred instead during routine walks to pick up groceries or meet a friend. About a week later, they menstruated for more than 30 days straight. After three weeks of bleeding, they went to see their doctor, who suggested that the tear gas had caused the disruption. “That’s what scared me,” Seamstress says. “They said that it seemed serious.” Seamstress didn’t have the means to purchase more menstrual products after their supply ran out, so they sewed their own reusable pads with the fabrics they had at home. They can’t afford a gas mask, a $40-230+ product which has become essential for many Minnesotans, either. At the height of protests, Seamstress avoided leaving the house. “A HIGHLY TENSE SOCIAL AND PSYCHOLOGICAL SITUATION”Staying home isn’t an option for everyone. Timothy Monko, a former post-doctoral researcher at the University of Minnesota, has investigated these chemicals, contributing to a 2021 paper scrutinizing the safety of tear gas. The research’s takeaway was clear: “We should not be using it without actually understanding its effects,” Monko says. Those findings were enough to scare him and his wife: They may want more children in the future, so his wife carried her gas mask everywhere when ICE officers were regularly facing off against local community responders this winter. Monko isn’t the only researcher to make similar conclusions. Public health expert Patricia Huerta has heard accounts of irregular menstrual cycles and miscarriages following tear gas exposure in Chile. The associate professor of public health and medicine at Chile’s University of Concepción published a 2023 paper focused on the 2019 social uprisings there, where police used crowd control agents during protests. She’s unsure whether chemical exposure alone is to blame for people’s symptoms—or whether it acts in combination with the trauma people experience during these law enforcement confrontations. “It’s a highly tense social and psychological situation,” Huerta says. “It’s quite stressful. It’s the smoke. It’s the smell. It’s a policeman pointing at you with a shotgun that you don’t know will shoot a tear gas canister or a rubber bullet.” Every researcher interviewed for this story agrees that there is a lot regulators still don’t understand about the long-term impacts of exposure to various types of chemical agents, but that they know enough to say with confidence that ICE’s recent use of tear gas and pepper spray isn’t safe. In the meantime, Seamstress is anxious over their next menstrual cycle. Asha, the street medic, remains available should her neighbors need her again. She’ll respond to emergencies however she can as long as her community is under attack. “Through all this, we’re just trying to meet the needs of our community,” she says. “We’re just looking after our neighbors….If it’s dropping off groceries or helping people pay rent, then it’s that. If it’s helping people who have been tear-gassed or pepper-sprayed, then we do that. We’re just helping in whatever way we can.”  ABOUT YESSENIA FUNESYessenia Funes is an environmental journalist focused on uplifting the voices of society's most oppressed. She publishes a climate-justice newsletter called Possibilities, and has been published in The Guardian, The Verge, Yale Climate Connections, National Geographic, New York Magazine, and more.  ENJOY MORE OF THE METEOR Thanks for reading the Saturday Send. Got this from a friend? Don’t forget to sign up for The Meteor’s flagship newsletter, sent on Tuesdays and Thursdays.
|
![]()
A Secret School for Girls
Inside the clandestine network of classrooms defying the Taliban in Afghanistan
By Jessie Williams
A group of teenage girls and young women gather in a nondescript room with pale walls, chatting and laughing. They have just finished their classes for the week and are about to head home. But they must leave one by one, so as not to draw any attention. If someone asks them where they have been, they say they were visiting the doctor. If they think someone might be on to them, the teachers move their classes to another person’s house. They leave their books at home. They must not be caught.
These girls live in Afghanistan, where education for girls beyond sixth grade is banned by the Taliban. They attend an underground girls’ school – one of five an Afghan NGO quietly runs across the country, with 28 teachers in different provinces providing free education to around 1,000 students, ranging in age from 13 to 45.
“I was very unhappy when the Taliban closed my school,” says Ada*, 15, who was in eighth grade when the Taliban returned to power on a hot summer day in 2021, following the withdrawal of U.S. and coalition forces. “I had depression.” The secret school she attends opened in the months afterward. “I feel better [now],” she says. “When I see the teachers and girls, I have power.”

As a new school year begins in Afghanistan, more than 2.2 million girls are currently out of school. But some of them are defying the ban. Over the past few years, classrooms have emerged in the shadows—cropping up in basements, living rooms and bedrooms around the country, away from the prying eyes of the Taliban, who have informants to catch people violating their strict codes. The schools use certain tactics to evade those informants, including staggering the timing of classes, so that some girls attend in the afternoon and some in the evening. If the girls think they’re being followed, they change their route. Madrassas, or religious schools, are still allowed, so if they are caught, they say they were going there.
The schools run by the NGO, which we can’t name for safety reasons, started through a network of trusted people in different communities. They cost about $60,000 to run each year, which a grant from the Frontline Women’s Fund, an initiative that supports women’s rights activists around the world, helps cover. One class was established and then another, and before long the network had blossomed into a web of clandestine schools, turning girls into what the Taliban fears most: educated women. “An educated woman changes the world,” says Laleh, 25, who teaches English at one of the schools. “An educated mother nurtures, trains, educates her kid. The kid changes the society.”
The Meteor spoke to the teachers and students over Zoom on the condition that we hide their identities. The stakes are high; if the Taliban ever found out about the schools, the teachers would be sent to prison, while the girls themselves could also face imprisonment and beatings. Despite the risks, the educators continue to teach. “When I was a girl, I studied chemistry. My father said ‘It's not safe to study.’ But I wanted to have a voice,” says Laleh. “When I teach the girls, they have the vocabulary to talk. It empowers me. When they learn, I think that I have done something in the world, that I didn't live a worthless life.”
Without education, she says, “our people don't even know how they should live and what their rights are…When half of our society is paralyzed, how can our country move forward?”
Since returning to power the Taliban has systematically eroded women’s and girls’ rights. Education for girls over sixth grade was the first to go, followed by barring women from university and nearly all forms of employment, then prohibiting them from playing sports, and even leaving the house without being completely covered and accompanied by a mahram or male guardian. The Taliban’s latest decree permits men to beat their wives as long as they don’t break any bones or leave open wounds.
The UN says that Afghan women are facing the most severe women’s rights crisis in the world, with many activists and human rights organizations calling it “gender apartheid”—a term meaning the systemic oppression, discrimination, and segregation of a specific group based on gender.

In January 2025, the International Criminal Court issued arrest warrants for the supreme leader and chief justice of the Taliban, accusing them of crimes against humanity for the persecution of women and girls. But nothing has been done to enforce the warrants. Even worse, the international community has begun to accept and normalize the Taliban as the de facto government, despite its draconian policies—like establishing embassies in Kabul, welcoming diplomats appointed by the Taliban, and inviting them to international summits.
Meanwhile, cuts to foreign aid budgets have meant dwindling humanitarian support for Afghanistan, and while the UN has continued its operations in the country, it faces major challenges—the main one being the ban on Afghan women entering UN premises, along with a 50 percent funding gap for UN work, which makes it difficult to provide services directly to women at a time when they desperately need it.
"Maybe they will arrest me and I go to jail. But I have to do this.”
Many Afghan women feel like the world has forgotten about them. Mariam, the 30-year-old executive director of the NGO that runs the schools, was a head teacher before the Taliban swept through the country. She says the international community should be doing more. “For five years girls and women can't go to school. It’s terrible. But nobody is doing anything,” she says. “Why aren’t the UN with us?”
Mariam says there are many women who are struggling financially now that they cannot work, and girls are being forced into early marriages. At the same time, recent clashes with Pakistan and war in neighboring Iran are exacerbating the already dire economic crisis.
For these girls, the school offers a glimmer of hope in an increasingly dark world, giving them the chance to forge their own futures. Bahar, a 19-year-old with a wide smile, was in 10th grade when the Taliban closed the schools. “When I come here I feel so excited,” she says, giggling. “I feel complete and confident.” Her favorite subjects are English and math, and one day she hopes to become a psychologist. “Education is very important to me. When girls use education, they can help their family.”
All of the girls’ families are supportive of them attending the classes, despite the dangers. “I feel happy because I improve my skills in this school,” says one student, Lama, 18. She especially loves art because it allows her to express her feelings, but wants to be a doctor when she’s older. “I want to help my people, always.”
Rehan, 21, a math teacher, says when she was her students’ age, “I had these opportunities as a student and I felt great. They should become what they want; I always teach them to become stronger.” Many of her students are vulnerable, she says, and so she makes sure to focus on their mental health. “When I come to class I ask them, ‘How was your day? How are you?’ Sometimes many of them don't have a good situation at home. First, I make sure they are safe, that they don't have any mental problems. Then I start to teach what I planned. I like to make the class a safer place for them.”
As the students and teachers talk, it becomes clear: These are much more than just schools. They also seem to be sanctuaries for women and girls to connect, laugh, and dream with friends. They are like a family, and Mariam, the head of the NGO, is the matriarch. She calls the students “my daughters” and sees supporting them as her responsibility. “It's a very big challenge,” she says. “We are afraid [of the Taliban finding out]. Maybe they will arrest me and I go to jail. But I have to do this.”
Despite the constant fear, they all still try to find joy – even if it’s fleeting. They dance and sing together when no one is looking. These girls are growing hope in the shadows; they’re creating cracks of light streaming through the darkness. “Sometimes we laugh, sometimes we cry,” says Mariam. “Maybe when the Taliban go, we will get our rights [back]. We want a new generation to feel peace.”
*All names in the piece have been changed to protect the subjects’ identity.

Jessie Williams is a freelance journalist focused on international affairs, humanitarian issues, and women’s rights, with work published in The Guardian, TIME Magazine, Foreign Policy, Al Jazeera, and more. She has reported from Syria, Lebanon, Iraq, and Ukraine, among other places.
Lipstick, Selfies, and Prosthetic Legs
Gaza is home to the world’s largest group of child amputees. A photographer documents the lives of two of those children, who are still healing and waiting.
By Eman Mohammed
Layan’s first request after her surgeries was simple: She wanted to wear dresses again.
Before the bombing, she loved how fabric moved when she spun, how a skirt could flare and turn an ordinary hallway into a stage. After she lost both of her legs in an Israeli airstrike on her home in Gaza, dresses became a negotiation with balance, stitches, and pain. Learning to walk again meant relearning her body, figuring out how to trust it enough to stand inside the clothes she missed.
Layan is not the only child from Gaza learning to adapt to life-altering injuries. The United Nations has reported that Gaza is now home to the world's largest cohort of pediatric amputees per capita, with more than 4,000 children losing limbs since October 2023.
Most of those children remain in Gaza, with little hope of being evacuated to receive rehabilitation in a safe environment. Since October 2023, organizations like HEAL Palestine have facilitated secure passage for 62 children to the United States through medical visas, but in August 2025, those visas were suspended for Palestinian passport holders. Extensions quietly disappeared. When treatment ended, the Trump administration required their return. HEAL Palestine pledged not to send any Palestinian child back into an active genocide, and since then, those who could not remain in the U.S. have been placed in temporary housing in Cairo, waiting for borders to open, for stability to return, and for a future that does not yet exist.
Layan, 14, was one of the children who were granted medical evacuation to the United States through Heal Palestine. She arrived in Chicago in March 2024, and her host family has navigated lawyers, deadlines, and a system built to send her back before she was ready, fighting to keep her in the country while she relearns how to walk on both prosthetic legs. For now, her healing continues there, and she’s back in school. She still wants to go back to Gaza, not out of nostalgia, but because it is the only place that feels complete. Return remains blocked under Israeli restrictions.
Rozan, 13, understands interruption in a different way. After her evacuation for treatment, she was sent back to Egypt to wait for the borders to open. She lives with another family sponsored by HEAL Palestine, a mom and a three-year-old from Gaza. Her time in Cairo stretched from temporary to indefinite. Rozan lost her leg and seventeen members of her family in a single Israeli airstrike. The number sits in the room even when no one says it, but she doesn’t perform grief. She draws, studies, argues about outfits before school, and laughs when clay collapses in her hands on a pottery wheel, then tries again.
Neither girl fits the story people want from them. They are not symbols of unmitigated triumph. Their days revolve around prosthetic fittings, therapy schedules, visa deadlines, and the long logistics of survival. Healing is technical work. It takes money, translators, housing, doctors, tutors, and adults willing to build a net strong enough to hold children who have already fallen too far. That net exists because a community refused to let them disappear.
HEAL Palestine and the families around it function less like charity and more like extended kin. Apartments become shared recovery spaces. Older children teach new arrivals how to balance on unfamiliar legs. Caregivers trade information about clinics, schools, immigration rules. The girls grow inside that ecosystem of attention. Their resilience is not solitary, it is built collectively, reinforced by people who keep showing up.
In the afternoons, Rozan’s apartment fills with ordinary noise. A ball skids across the tile. Someone shouts. Someone laughs. Inside that chaos is the thing policy could not erase: children insisting on motion, and a community answering by making sure they never have to move alone.
Click on the images below to view the photo gallery.

Eman Mohammed is an award-winning Palestinian photojournalist from Gaza and Senior TED fellow. Her work has been featured in Le Monde, VICE, The Washington Post, The Atlantic and more.
She Fled Fear—and Found It Here
A woman who escaped danger in Afghanistan reflects on what life is like under ICE.
By Lima Halima-Khalil
I drop my three-year-old daughter off at library classes every morning. The library is two minutes from our home in Ashburn, Virginia. Each time, the same thought crosses my mind: Do I have my ID on me? Will my driver’s license be enough if I am stopped?
It is highly unlikely that I will encounter ICE on a two-minute drive to the library. Ashburn isn’t exactly an ICE hub. And yet my fear is constant, embodied, and real. And by the way, I am an American citizen.
I grew up believing America was a mighty country, one so powerful that the rest of the world stood intimidated by its strength. When I first came to the United States in 2006 for an education program from Afghanistan, a country still at war, the vastness of this place revealed itself not only in its size, but in the generosity of the people I met. After that, America became a place I always returned to. I have been part of the American education system since 2010, returning several times for various degrees. I’ve witnessed multiple presidential elections and participated in the most recent one as an American citizen myself.
But after all these years, one lesson about my new home stands out above the rest: This country is led, shaped, and sustained by fear. Outside this country, nations tremble at the military and economic power of the United States, but inside it, people live as though danger is always lurking.
Fear raises money and sustains campaigns. Fear keeps people glued to screens and locked into cycles of outrage. Fear sells guns, justifies surveillance, expands borders and prisons. Much of this fear is not grounded in lived reality but manufactured and amplified by politicians who rely on it to govern. Fear spills into kitchens, sidewalks, classrooms, and moments meant to be ordinary and human.

One of the most brutal tools in this ecosystem right now is ICE. Raids, detentions, and aggressive enforcement practices operate not simply as immigration policy, but as a mechanism of fear, reminding entire communities that their sense of belonging is fragile and conditional. ICE does not need to be everywhere to be effective. The possibility of its presence is enough.
This pervasive fear turns ordinary routines into sites of anxiety. I remember hesitating before offering to share our Thanksgiving meal with our nosy white neighbor, suddenly gripped by thoughts I never imagined I would carry. What if he calls the police on us and claims I was trying to poison him? What if kindness itself is misread as a threat, or hospitality as danger?
Afghans discovered how quickly they could become the “other,” regardless of their sacrifices, their loyalty, and their love for this country.
I recognize these impulses, because fear is not new to me. I lost my school, my home, my loved ones, and eventually my country because I wanted freedom from fear. Millions of Afghans had believed in democracy when America promised it to us for 20 years, until the United States withdrew from Afghanistan in 2021. We voted, we hoped, we worked alongside our American partners for a shared dream, but that freedom never came. In 2020, when my 24-year-old sister was killed by the Taliban in an IED attack in her car, that truth became undeniable. I understood then that Afghanistan was no longer safe, and that realization is what led me to come to the United States permanently.
When the Taliban returned to power in 2021, many Afghans, including members of my own family, were evacuated and brought into this country by our American allies. They arrived in this country under extremely harsh circumstances, believing they would find dignity, safety, and a chance to contribute. Instead, they discovered how quickly they could become the “other,” regardless of their sacrifices, their loyalty, and their love for this country.

I was reminded of this again in November of last year, after a man from Afghanistan, who had been trained and worked for the CIA in his country, shot two National Guard members in Washington, D.C. Overnight, an entire community began to be seen, once again, as terrorists. Instead of a careful and humane conversation about mental health, trauma, or resettlement failures, the Trump administration halted all immigration from Afghanistan and pledged to re-examine green card holders from 19 countries. Afghans, many of whom fled the very forces America claims to oppose, were once again forced to prove their innocence.
This is how fear functions. It identifies a moment of tragedy, strips it of context, assigns collective guilt, and converts pain into political currency.
For a long time, I believed that fear in this country belonged primarily to people of color, that violence was uneven, predictable, and racialized. Then the killings of Renée Good and later Alex Pretti shattered that belief. They forced a painful realization that in today’s America, no one is safe, not five-year-old Liam Conejo Ramos, not women citizens like Dulce Consuelo Díaz Morales and Nasra Ahmed, not elderly citizens like Scott Thao or longtime residents like Harjit Kaur, not white Americans, either.
Lately, I have felt fear settle into my own body in a way I did not expect. I realized I had been going to sleep holding fear, living with the same quiet dread that so many people here carry without ever naming it. One night, I caught myself thinking, almost with disbelief: Congratulations, Lima, you are an American now.
But it does not have to be this way. Americans deserve more than this constant weight of dread, clinging to them like a second skin. We deserve a country where fear is not the engine that keeps the system running, where safety is not promised to some by threatening others, and where power is not sustained by keeping people afraid.

Lima Halima-Khalil, Ph.D., is the program director of the “I Stand With You” campaign at ArtLords, a collective she co-founded, where she mobilizes global awareness against gender apartheid in Afghanistan. Her research explores youth resilience amid violence and displacement. Her writing has appeared in Foreign Policy, TRT World, and academic publications.
Chrissy Teigen: "This is what care looks like"
Against a landscape of shrinking reproductive freedom, the TV personality and author visits a Tennessee clinic that offers both birth and abortion care
Tomorrow marks the 53rd anniversary of the Roe v. Wade decision. More than half a century later, in a country that no longer grants the freedom that that ruling declared, it’s easy to get mired in the onslaught of harrowing news about our bodies and our lives. But everywhere, there are warriors who keep doing the work of caring for pregnant people, and they are not mired. They are moving forward, every single day.
TV personality and best-selling cookbook author Chrissy Teigen has herself helped to humanize reproductive healthcare. She has spoken about her own experience having a lifesaving late-term abortion; visited the Feminist Center for Reproductive Liberation, a clinic in Georgia, in 2024; and then discussed her experiences with Vice President Kamala Harris during the 2024 presidential campaign. “I started crying once I saw this beautiful mural of butterflies above the operating suite” at the Feminist Center, Teigen told Harris at the time. A doctor there “looked me in the eye and she said, ‘You could have had butterflies.’”
Then, in 2025, The Meteor traveled to Tennessee with Teigen on another visit—one that shows that everyone deserves butterflies, and that you can’t talk about abortion care without talking about maternal care. CHOICES Center for Reproductive Health, a Memphis-based clinic, provides the full spectrum of care for people who can get pregnant. “All pregnancies are different,” says Jennifer Pepper, CEO and president of CHOICES. That’s why the center provides everything from midwife-assisted births to high-risk pregnancy care to prenatal classes—and, since abortion was banned in the state in 2022, abortions in their sister location three hours away in Carbondale, Illinois. (Pepper says CHOICES is the only nonprofit in the country where both birth and abortion take place. And after Dobbs, “we could not stomach the idea that [abortion] patients wouldn’t have anywhere to go,” she says.)
“Every single woman deserves that level of care in America,” Teigen says. “This is what care looks like—people listening to you, and treating your body and your choices with dignity.”
Teigen was moved by how the clinic felt so “open and welcoming and airy and light,” with a “sisterhood” that was far from “the coldness” of her own hospital experience. “It never crossed my mind that I could give birth on all fours, or be in a tub at a birthing center,” she said. She saw a better way to give abortion care, too. When Pepper told Teigen she got her start at CHOICES as an abortion doula, Teigen said, “I can’t tell you how much I would have appreciated an abortion doula,” someone to explain “what was happening with my body.”
Tennessee also has the highest rate of maternal mortality in the country—and so access to supportive birth care can mean the difference between life and death, particularly for Black women. One Black woman in the prenatal class, Jasmine, recalled a conversation with her doula at CHOICES that started with a heartbreaking wish—“First off, I don’t want to die”—and ended with her having a “beautiful experience” delivering her baby.
“Every single woman deserves that level of care in America,” Teigen says. “This is what care looks like—people listening to you, and treating your body and your choices with dignity.”
Producer/director/editor: Emily Murnane
Producer: Rachel Lieberman
Director of photography: Mary Gunning
Audio: Stacia Gulley
Production assistant: Dindie Donelson
Production assistant: Nola Madison
Post producer: Annie Venezia
Graphics: Bianca Alvarez
Produced with support from Pop Culture Collaborative, as part of the United States of Abortion series.
Syria's Mothers are Fighting to Rebuild Their Homes
One year after the end of a long war, they tell journalist Tara Kangarlou what coming home has really been like
By Tara Kangarlou
“There are very few mothers here who haven’t lost a child or a spouse, and very few children who haven’t lost a mother or a wife,” says 62-year-old Khadijah as she sits on the floor of a heavily bombed building—flattened, except for the one room where she now lives with her 75-year-old husband, Khaled. Like most of her neighbors, Khadijah, her husband, and her children—previously displaced across Syria and neighboring Lebanon and Turkey—are now returning to their devastated hometown of Zabadani, wondering how to pick up fragments of a life uprooted.
The nearly 13-year-long war in Syria is known as one of the worst humanitarian crises of the 21st century. According to the United Nations High Commissioner for Refugees, the conflict displaced more than 13 million Syrians, including the six million people who fled to neighboring countries. For years, the war functionally dismantled the country’s healthcare and infrastructure and robbed an entire generation of school-aged children of their childhood and education—losses that ripple through every fabric of Syrian society today. The UN Human Rights Office has documented over 300,000 civilian deaths, with some estimates approaching half a million. Multiple mass graves have been found across the country, and Bashar al-Assad’s deployment of chemical weapons in Ghouta and Duma against his own people marked the deadliest use of such agents in decades.
This month marks a year since the fall of Bashar al-Assad, and over that time, millions of Syrians have been adjusting to their newly liberated reality. More than four million have made their way back to their villages across Syria—their homes reshaped by years of siege, bombardment, and civil war. In Zabadani, Eastern Ghouta, Madaya, Duma, and other hard-hit regions across the country, mothers—like Khadijah—are navigating these losses firsthand as they work to restore a semblance of stability for their families.

It should be a time of celebration, but for those living among the remnants of destruction, grief is pervasive. “Before the war, I would always wear white, but ever since the first death in our family, I’ve not taken off my black scarf,” Khadijah says. “I continue to be in mourning,”
Like so many others in Syria’s Zabadani region, Khadijah and her family hail from generations of experienced, hard-working farmers. But the land, once celebrated for its apple orchards, vineyards, and lush farmland that helped feed Damascus, endured one of Syria’s longest and most punishing sieges. Between 2015 and 2017, barrel bombs, airstrikes, and artillery shells rained down, destroying irrigation systems, flattening farmland, and contaminating the earth with heavy metals, TNT, and fuel residues. The blockade also choked off agricultural inputs—seeds, fertilizers, and clean water, leading to the collapse of a once-thriving rural economy.

“We’d feed an entire town with our fruits and vegetables, but now, we barely have enough to feed our own family,” says Khadijah, whose grievances are evident when you visit her farm, where the soil is depleted and infrastructure destroyed.
“The only people whose farmland was spared were the people who cooperated with the Assad regime,” Khadijah explains. “We’re grateful to be alive, and we will rebuild, even though right now, we just don’t know how.” Later, she recalls the harrowing days in 2015 when she, her two daughters, and her then two-year-old grandson, Ammar, were displaced to nearby Madaya as the Assad army besieged Zabadani. Soon, those under siege in Madaya were facing severe food shortages and starvation under a blockade imposed by Assad’s forces and his allies Russia and Iran-backed Hezbollah.
“Ammar’s father [my son-in-law] was just killed…when we were forcefully moved to Madaya,” she says. “We had so much grief. “For the nearly two years that followed, we had nothing to survive on except rationed sugar, bread, and at times animal feed and grass.”
It wasn’t until 2017, following months of siege, that Khadijah and her family were relocated to opposition-held Idlib where they continued to live in displacement with little means to support the family.
Now 22, Ammar is studying to be a medical technician in Idlib—a city that remained the only lifeline for hundreds of thousands of displaced Syrians during the war. Visiting his grandparents in Zabadani, he brings in freshly made Arabic coffee and sits next to his grandmother and 37-year-old uncle Omar, who lost an eye in the war. Both men look at Khadijah with deep respect and endearment. “Every single mother in Syria has suffered tremendously, including my own mother and my grandmother; but we are of this land, and we’re happy to be back,” said Ammar.
The Flowers Still Bloom
Across Syria, the devastating impact of warfare is as environmental as it is emotional.
Just an hour’s drive from Damascus, 35-year-old Hiba walks through her hometown of Duma in Eastern Ghouta, stopping at a perfume shop to buy rose-scented oils—a defiant joy after surviving years of siege, bombardment, and chemical attacks. “Everything above ground was destroyed,” she says, recalling giving birth during the war in a half-collapsed clinic with no medicine, water, or electricity. Today, Hiba calls her 7-year-old daughter, Sally, her best friend and the person who makes life meaningful. “She loves riding her scooter and wants to be a pharmacist,” Hiba shares.

During the war, inspired by her family’s struggles caring for her younger brother with Down syndrome, Hiba began working with children with special needs—a profession she continues to this day, despite her own personal battles.
“People were disconnected from the world,” she says, pointing to what once was her house—a collapsed building lying under the weight of repeated barrel bombs and artillery strikes. “Our country is destroyed, but we mustn’t forget what happened to us. Our children must remember everything—so it doesn’t happen again.”
Both Zabadani and the Eastern Ghouta regions stand as stark evidence of how siege warfare and chemical weapons became tools of collective punishment—obliterating not just lives, but the ecosystems and livelihoods that sustained millions of ordinary civilians, including mothers, who are now searching for hope amidst rubble.
Back in Zabadani, 35-year-old Lana—a mother of two toddler boys—walks the grounds of her grandfather’s house and what was once her safe haven as a child.. She is a psychologist who has recently returned to her flattened town after years of life as a refugee in Lebanon. Today, along with her husband, she’s back “home,” doing what she once dreamed of doing for her own people and community.
“This is my grandfather’s home. My daddy grew up here,” she says. “We used to play here as children.”
The building’s walls are pocked with shrapnel holes and its ceilings blown down into rubble, but as we climb up and walk into the remnants of the house, she suddenly turns around, tearing up. On a half-collapsed wall, a faint drawing survives—painted decades ago by Lana’s father as a child, and depicting a red house surrounded by trees and a bright blue lake—the last fragile trace of a family’s life before war.
“My daddy was an artist. I have to tell him this is still here.” She looks at the flowers growing from underneath a pile of stones and smiles: “See, even in the middle of this destruction, we still have flowers bloom. There is hope, Tara. We are here.”


Tara Kangarlou is an award-winning Iranian-American global affairs journalist who has produced, written, and reported for NBC-LA, CNN, CNN International, and Al Jazeera America. She is the author of The Heartbeat of Iran, an Adjunct Professor at Georgetown University, and founder of the NGO Art of Hope.
"We're Being Robbed of Time"
Two women share what it was like to lose their husbands to "self-deportation."
By Anna Lekas Miller
Ordinarily, Julie is a night owl. She is used to staying up late while her husband, Neftali, whom she affectionately calls “Nef,” goes to bed early to wake up for his construction jobs.
Even these days, “I find myself tiptoeing around at night, trying to be quiet,” she says. “Then I realize he isn’t there.”
Neftali didn’t pass away—in October, he made the difficult decision to “self-deport” to Mexico, leaving Julie, a U.S. citizen and business owner, behind in Newark, New Jersey. And like a growing number of families in Trump’s America, they are now living separated by a border, wondering what they have to do to find their way back to each other.
Julie, now 47, and Neftali, 45, first met through friends in 2008 and started dating in 2011. Back then, she didn’t think it was a big deal that he didn’t have papers. But when Trump first came to office in January 2017, they started getting nervous. The two went to City Hall to tie the knot, just to be safe. “We didn’t want to take any chances,” she says.
But when they went to adjust Neftali’s status, they were slapped with a rude awakening. Even as a U.S. citizen, Julie couldn’t sponsor Neftali—long before they met, he had crossed the border twice, and because of a piece of Clinton-era legislation, this meant that he was ineligible for a green card. At the time, they decided to do what they always do—look over their shoulder and stay away from police. But as Trump’s second crackdown on undocumented immigrants began, and they started to hear more stories of people being detained and even disappearing, Julie and Neftali began to reconsider their lives in the United States.
When the couple finally decided it was time for Neftali to leave the U.S. last month, Julie traveled with him. “I spent five days with him in Mexico, and it was one of the most painful, but exhilarating experiences.” Julie says. The moment there was no longer a threat of Neftali being arrested, she adds, both of them felt immense relief.

It is difficult to know precisely how many people have self-deported from the United States. The Department of Homeland Security claims that 1.6 million individuals have done so using the CBP Home app, but this number has been disputed.
Julie and Neftali represent one of 4.5 million “mixed-status” households across the country. Some of these households include a U.S. citizen married to someone without papers; others include children born in the United States to undocumented parents. All undocumented individuals are vulnerable now, but statistically, it is men who are more frequently targeted during ICE raids; when they are forcibly removed from their families, be it through arrest or self-deportation, their spouses and children are left behind to navigate a cruel system.
“We’re being robbed of time together,” Julie tells me. “When I’m having a bad day or a bad moment, I can’t feel him close like I do when he’s here.”
“We weren’t really living.”
Several states over, in North Carolina, Jenni Rivera, 54, and her husband, Fidel, 48, share a similar story. Jenni is a high school math teacher; Fidel, an electrician. They have two children together and met salsa dancing almost twenty years ago. “It was like the beginning of any relationship—we just couldn’t get enough of each other,” Jenni recalls.
Even though Fidel had been living in the U.S. without papers when they met, Jenni assumed that she could fix it through marriage. But when they went to an attorney, they learned that he would likely be barred from re-entering the country for 10 years if he tried to adjust his status. “At the time, we had an infant,” she tells me. “There was no way that I was going to separate my spouse from his daughter for 10 years.” So Jenni and Fidel accepted that they would continue to live in the shadows.

“We didn’t go anywhere [that] we couldn’t drive [to],” she remembers—boarding a plane and having IDs scrutinized by TSA agents felt too risky. That meant no more trips to Florida to see her family, and no vacations that weren’t within a short drive of their home in North Carolina. In the summer of 2024, Jenni took their daughters—both U.S. citizens by birth—on a road trip across the country, but without Fidel, it felt empty. “I knew he would love the prairie dogs,” she laughs, recalling a stop in South Dakota. “He would be making up stories about them, having ridiculous conversations with them, telling the girls stories from when he used to be a rancher.”
Over the years, it felt like the box they lived in was getting smaller and smaller. Even though they had all of the hallmarks of a good life—stable jobs, a nice house, two wonderful children—the constant threat of deportation made her painfully aware of the fact that she could someday be on her own.
“I could feel the walls closing in on us,” she describes. “We were living, but we weren’t really living.” Still, a lawyer had told Jenni that if Fidel ever got arrested, she could bail him out, and they would eventually have their day in court, where an “extreme hardship” provision in immigration policy might allow Fidel to stay in the United States. That gave her hope, but then, in September of this year, the Board of Immigration Appeals took this option away. “They blocked the one chance I had to fix anything.”
As time wore on, too, things got scarier. Detention centers, like Alligator Alcatraz, started popping up, and Jenni realized that Fidel might not just get deported—he could be detained for months, or disappear entirely. “My husband is such a good human. I did not want him to be in any of these places that we were hearing about,” she says. “I couldn’t live with myself. I wouldn’t be able to face my kids again.”
So, on October 10th, they celebrated their 17th wedding anniversary. They carved pumpkins and ordered pizza with their girls. Then Jenni helped Fidel pack for his flight to Mexico.
“It was really sad at the airport,” she tells me. “But I’ve been staying busy. I think it’s really going to hit in the quiet moments.”

"Our plans look a little different..."
One of many frustrations that Jenni and Julie share is the amount of apathy towards immigrants that they witness among other Americans. “It isn’t just about deportation anymore,” Julie says. “It’s about detention and people disappearing and making money on detained bodies. I’m disappointed more people aren’t outraged.”
“They are destroying families,” Jenni adds. “I can’t understand what these people did that was so bad that you would want to rip the foundation of their life apart.”
Since Fidel left for Mexico, Jenni has been focusing on helping her oldest daughter with college applications. “I know if they want to come to me, they’ll come to me,” she tells me when I ask how they’re doing. “I don’t want to burden them.”
Meanwhile, Julie is continuing to support other mixed-status families through American Families United, an organization that advocates for legislation like the Dignity Act, which would allow undocumented immigrants to regularize their status provided they pass a criminal background check and pay any taxes that they owe. She’s also looking forward to the next time that she can visit Neftali in Mexico—and hopes to eventually move there.
“We talk every night,” she says. Sometimes, they reminisce about the past; mostly, they look forward to the future. While they once thought this would be in the United States, now they know that this will be in Mexico.
“Our plans look a little bit different than how we thought they would look,” Julie says. There are logistical issues. Neftali had been paying for his niece’s education, which is going to be more difficult when he’s earning in pesos instead of dollars. Julie is working on finding a way to pivot her business to something that she can do from Mexico.
“I don’t want any more time to be stolen from us,” she adds. “We’re going to work as hard as we can, so we can have a beautiful future like we always planned.”
“I feel a sense of freedom,” she says. “It’s just not in the United States.”

Anna Lekas Miller is a writer and journalist who covers stories of the ways that conflict and migration shape the lives of people around the world. She is the author of the book Love Across Borders and runs a newsletter by the same name. Follow her on Instagram: @annalekasmiller.
"A revolution has begun. There is no going back."
On the anniversary of the Beijing women’s conference, a blueprint for a brighter future
Thirty years ago this month, women from around the world gathered for a conference that made history and, as it turned out, would not happen again. The 1995 UN Fourth World Conference on Women in Beijing was a monumental moment for activists and world leaders who came together to “answer the call of billions of women who have lived, and of billions of women who will live,” as the first female Prime Minister of Norway, Gro Harlem Brundtland, put it at the time. It’s the meeting at which then-First Lady Hillary Rodham Clinton, building on years of women’s organizing, famously said, “Women’s rights are human rights,” which made global news because it was (and apparently remains) a radical perspective.
The journey to the conference—which is documented in a new multimedia project from the United Nations Foundation and co-produced by The Meteor—was two decades long, with previous meetings held in Mexico City, Copenhagen, and Nairobi. Beijing itself was the largest women’s rights gathering at that point in history, with a massive audience of 45,000 people invested in building a better future. Pulling it off was no small task, but the leaders charged with doing so were more than up to it. Among them was the inimitable Gertrude Mongella of Tanzania, the Secretary-General of the conference, who later became known as Mama Beijing. “A revolution has begun,” she said during a closing speech at the Conference, “there is no going back.”
Mongella was a key player in producing the Beijing conference’s most significant document: The Beijing Declaration and Platform for Action—which remains the most comprehensive blueprint for gender equality and women’s rights ever created. It wasn’t just a wish list; 189 countries committed to it in Beijing. It demanded women’s inclusion in government and policymaking; economic policies built with gender in mind; the understanding that violence against women is a human rights violation; and was also one of the first international agreements to demand that governments complete a thorough analysis of how climate change and industrialization had affected women. From the Platform: “The continuing environmental degradation that affects all human lives has often a more direct impact on women…Those most affected are rural and Indigenous women, whose livelihood and daily subsistence depends directly on sustainable ecosystems.”
You probably know how this ends: While some of the Platform’s key goals have been achieved—women’s representation in government, for instance, has risen—many have yet to be fulfilled, 30 years later, not because of an absence of activism, but because of global backlash and competing priorities. But the women at the forefront of global change remain motivated. When asked what the next global feminist conference should focus on, Nyasha Musandu of the Alliance for Feminist Movements put it this way: “We must dare to dream bigger, disrupt deeper, and build bridges across movements. The fight for justice is not just about breaking barriers—it’s about reimagining the world itself.”